Diabetes, a chronic condition affecting millions globally, not only alters lifestyle but also brings about unique health challenges. Among these, wound healing is a significant concern. For diabetics, a simple wound, if not properly managed, can escalate into a severe complication, sometimes leading to dire consequences like amputations or life-threatening infections.

Understanding the criticality of proper wound care for diabetics is not just a matter of health literacy; it’s a vital component of effective diabetes management. This blog post delves into why wound care is paramount for diabetic individuals and how it can be optimally managed.
The Challenge of Wound Healing in Diabetes
Diabetes impacts wound healing due to several factors, including poor blood circulation, nerve damage (neuropathy), and a weakened immune system. These factors collectively slow the healing process, making wounds susceptible to infection and complications. Given these risks, diabetic patients require specialized care for even minor injuries. Mobile Wound Care Experts play a crucial role in this scenario, providing tailored wound care services that cater to the unique needs of diabetic patients.

Photo Credits: Photo by Tara Winstead: https://www.pexels.com/photo/close-up-view-of-band-aids-on-blue-surface-7722865/
The Role of Blood Sugar Control in Wound Healing
Blood Sugar Management: The cornerstone of effective wound care in diabetics is maintaining optimal blood sugar levels. High glucose levels can impair the body’s natural healing process and increase the risk of infections. Regular blood sugar monitoring and adherence to prescribed diabetic medications are crucial to promoting wound healing.
Regular Inspections and Early Intervention
For diabetics, it’s essential to inspect their feet and other prone areas daily for cuts, blisters, or sores. Early detection of wounds is critical in preventing complications. If a wound is spotted, seeking medical attention promptly is imperative. Delayed care can lead to infections or non-healing wounds that can have severe consequences.
Best Practices in Diabetic Wound Care
Cleanliness and Protection
Keeping the wound clean and protected from further injury is paramount. Gently cleansing the area with mild soap and water removes debris and reduces the risk of infection. Dress the wound with sterile bandages, which protect it from environmental contaminants and maintain a moist environment conducive to healing.
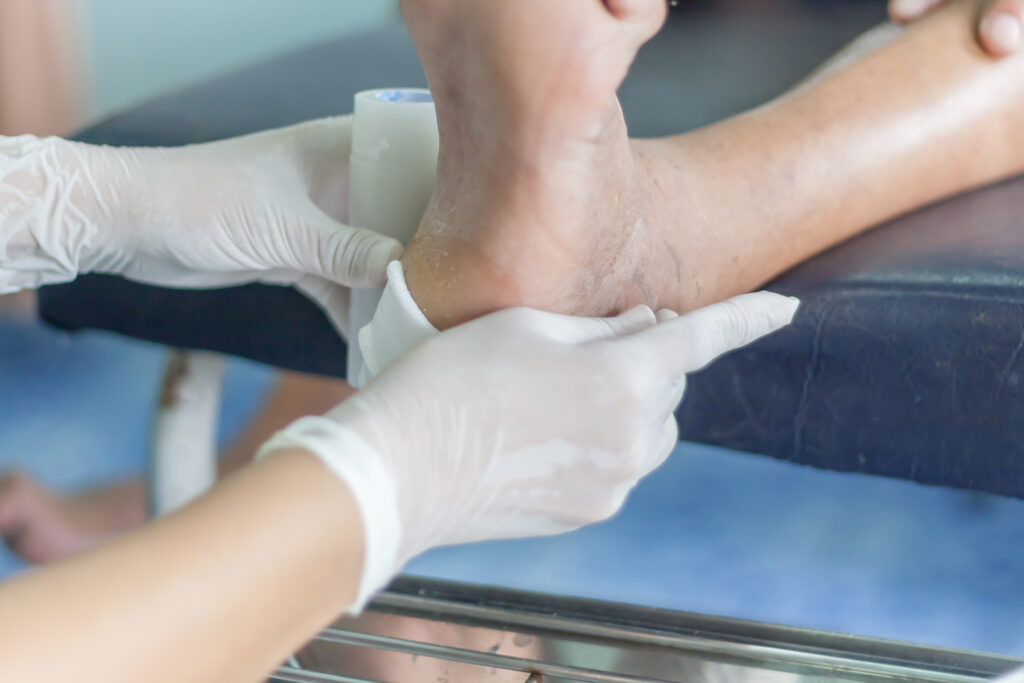
Picture credits: https://www.nih.gov/news-events/nih-research-matters/poor-immune-response-impairs-diabetic-wound-healing
It’s crucial to avoid harsh chemicals or antiseptics unless specifically recommended by a healthcare provider, as these can irritate the wound or delay healing. Regularly changing dressings and inspecting the wound for signs of infection, like increased redness, swelling, or a foul odor, is key. It’s important to consult a healthcare professional immediately if any such signs are noticed.
Appropriate Dressings and Offloading
The choice of dressing can greatly influence the healing process. Highly absorbent dressings are ideal for wounds with excessive drainage, while hydrogels can benefit drier wounds by providing necessary moisture. Foam dressings, which are soft and absorbent, can be particularly comfortable for patients. In foot ulcers, offloading is essential and can be achieved through special footwear, such as diabetic shoes or custom orthotics, or devices like crutches or wheelchairs.
Offloading helps distribute weight away from the wound, reducing pressure and friction, which are critical in preventing further injury and promoting healing. Regular follow-up with a healthcare provider ensures the wound care regimen is effective and adjusted as the wound heals.
Lifestyle Modifications
Healthy lifestyle choices are critical in wound healing, especially for diabetics. A balanced diet rich in vitamins and minerals, particularly Vitamin C, Zinc, and proteins, supports the body’s repair mechanisms. Staying well-hydrated is essential as it aids in maintaining skin elasticity and promotes efficient blood circulation, which is necessary for wound healing.
Smoking cessation is vital; smoking constricts blood vessels and impairs oxygen and nutrient delivery to the wound site, significantly slowing the healing process. Similarly, controlling alcohol consumption is important as excessive alcohol can weaken the immune system and delay healing. With a doctor’s approval, regular exercise can enhance blood flow and improve overall health, further aiding the healing process. These lifestyle modifications and careful wound management create an optimal environment for wound healing in diabetic patients.
Conclusion
Effective wound care for diabetics is not a standalone task but an integrated part of diabetes management. It requires vigilant monitoring, rapid response to injuries, and adherence to a comprehensive care plan. The collaborative effort between healthcare providers, such as Mobile Wound Care Experts, and the patient is crucial. Empowerment through education about the importance of wound care and the adoption of healthy lifestyle practices can make a significant difference in the lives of diabetic patients. With the right care and attention, the risks associated with diabetic wounds can be greatly minimized, leading to better health outcomes and an improved quality of life. Remember, in diabetic care, every wound deserves your attention.

David Johnson is a versatile content writer known for his ability to breathe life into words and create engaging narratives on diverse subjects. With a passion for effective storytelling and a keen eye for detail, David crafts content that resonates with readers and sparks their curiosity. He is dedicated to delivering high-quality, informative, and enjoyable content, making him a respected voice in the digital landscape. Beyond the keyboard, David enjoys exploring the outdoors, immersing himself in literature, and finding inspiration in everyday experiences.






Loading…